Hot flashes: Causes, symptoms, & treatments
If you’re in your late 40s or 50s, you may have found yourself asking, “Why am I suddenly overheating?” You’re not alone. Hot flashes are one of the most common symptoms during perimenopause and menopause. They’re completely normal, but that doesn’t make them any less disruptive or frustrating.
Hot flashes might be a normal part of menopause, but it doesn’t mean you have to “just tough it out.” We’ll help you understand why they’re happening and offer some practical tips to reduce their intensity and help you start feeling more like yourself again.
What are hot flashes in perimenopause and menopause?
Hot flashes, also known as vasomotor symptoms, are one of the most recognizable signs of perimenopause and menopause. The sudden surges of warmth can leave your skin flushed, your heart racing, and your patience tested. Nearly 80% of women experience them at some point during perimenopause and menopause. They’re a completely natural response to changing hormones, but that doesn’t make them any less uncomfortable.
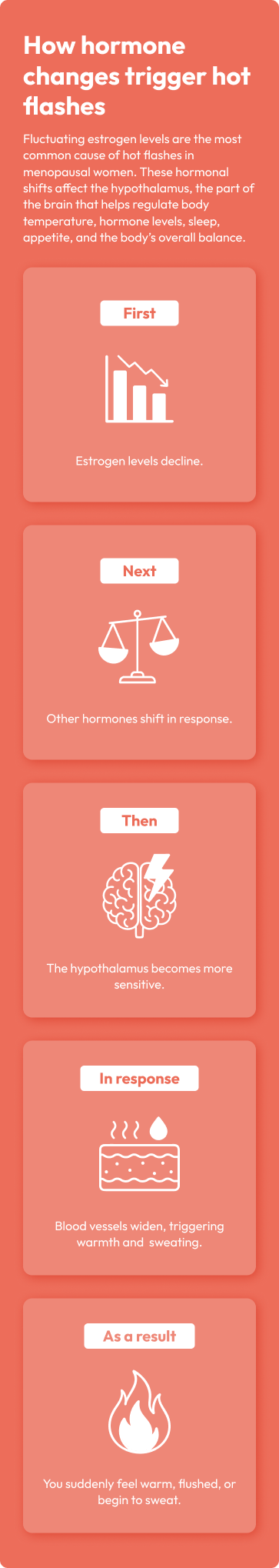
As estrogen levels fluctuate, the hypothalamus (the part of your brain that helps regulate body temperature) becomes more sensitive. Small shifts in body temperature can trigger an exaggerated cooling response, sending blood rushing to the skin’s surface and causing sweating, redness, and that all-too-familiar heat wave.

When do hot flashes start?
Hot flashes and night sweats (hot flashes that occur while sleeping and, commonly, disrupt your ability to get a good night’s rest) often begin in perimenopause, the transition that typically starts in a woman’s 40s but can begin earlier, sometimes in the 30s. They may continue well into post-menopause, gradually easing over time.
- 40s: Hot flashes and night sweats may start as hormone levels fluctuate.
- Mid-40s to early 50s: Menopause typically occurs, defined as 12 months without a period. Hot flashes often peak in the first few years after this transition.
- Late 50s and beyond: While symptoms usually reduce, they can persist for several years for some women.
“Hot flashes begin in perimenopause and can persist for 7–10 years,” mentions Dr. Sherry. “Since perimenopause occurs up to 10 years before the menopause transition, many suffer from hot flashes for longer periods of time, depending on the time perimenopausal symptoms appear.”
The good news? They often become less frequent and less intense over time.
What are the signs of hot flashes?
No two women experience perimenopause or menopause the same way, but hot flashes often share some hallmark sensations:
- A sudden wave of warmth in the face, neck, or chest
- Flushed or reddened skin
- Profuse sweating
- A racing heartbeat or mild anxiety
- Chills once the warmth subsides
- Disrupted sleep when symptoms occur at night (aka night sweats)
Episodes usually last between one and five minutes, but their frequency can range from occasional to several times a day.
While hot flashes often occur without warning, some women feel an anxious “aura” just before one begins, or chills afterward. Most last about five minutes, but in the moment, they can feel much longer.
What causes hot flashes?
Hot flashes are tied to fluctuating estrogen levels. During perimenopause and menopause, your hormone levels fluctuate wildly, and your estrogen levels drop. Estrogen helps your hypothalamus regulate body temperature. When estrogen levels rise and fall unpredictably, your hypothalamus can misfire. It thinks your body is overheating and signals you to cool down by opening blood vessels and making you sweat.
When hormones spike and drop unexpectedly, as they do during perimenopause and menopause, it’s difficult for your body to regulate its temperature. This leads to sweating and those sudden and almost electric heat sensations. That’s why hot flashes feel like a sudden surge of heat, almost like your body has flipped on a switch.
“Hot flashes are one of the most common symptoms of menopause, affecting up to 80% of women, with some women experiencing more than 10 a day,” explains Dr. Sheryl Ross (Dr. Sherry), Chief Medical Officer of Women’s Health here at QuickMD. They tend to last an average of five minutes, but, as Dr. Sherry notes, “Everyone experiences hot flashes differently; some are less explosive or disruptive, but not for others.”
She adds, “It’s important to remember everyone has an individualized experience going through the perimenopause and menopause transition, so your experience can be a lot different than your closest girlfriends.”
Treatments for hot flashes during perimenopause and menopause
Hot flashes are a normal part of menopause, but “normal” doesn’t mean you have to suffer through them. Treatment depends on how severe and disruptive your symptoms are.
Medical treatment options
Menopause hormone therapy (MHT)
Menopause hormone therapy (MHT), sometimes referred to as hormone replacement therapy (HRT), is the most effective treatment for hot flashes. It works by restoring declining estrogen levels and stabilizing temperature regulation in the brain.
Studies show MHT can reduce hot flash frequency and intensity by up to 75–80% for many women. It can also improve related symptoms such as sleep disturbances, mood changes, and vaginal dryness.
Therapy is tailored individually depending on your health history and symptoms. MHT is available in various forms, including oral tablets, patches, gels, sprays, or vaginal applications.
While hormone therapy isn’t suitable for everyone, most healthy women under age 60 or within 10 years of menopause onset are good candidates. Your QuickMD doctor can help evaluate your risks, benefits, and ideal formulation.
Nonhormonal medications
For women who can’t or prefer not to use hormones, several prescription options are available:
- SSRIs/SNRIs (e.g., paroxetine, venlafaxine): Can reduce hot flash frequency by up to 60%.
- Fezolinetant: A new FDA-approved medication that blocks neurokinin B signaling, a key pathway in triggering hot flashes, reducing frequency by over 60% in clinical trials.
- Gabapentin or clonidine: Can lessen the frequency or intensity of hot flashes, particularly when taken at night.
Your doctor can help determine whether these options fit your health needs and other medications.
Over-the-counter therapies: do they work?
Many women explore natural supplements and herbal remedies. Some of the most common include:
- Black cohosh and red clover: Plant-based compounds with estrogen-like effects.
- Soy or flaxseed: Contain phytoestrogens that may help mild symptoms.
- Evening primrose oil and dong quai: Used traditionally for menopause support, though evidence is limited.
While these may help mild cases, results vary, and safety can depend on your overall health and medications. Always consult your doctor before starting any supplement.
Lifestyle and relief strategies
Wear breathable layers
Choose light, breathable fabrics like cotton or moisture-wicking blends. Layers make it easy to adjust quickly if a flash starts. Some women even keep a small fan handy to get relief on the spot. For an even more fashion-meets-function approach, Dr. Sherry suggests, “There are many cooling products on the market that may ease the disruption of hot flashes. Cooling scarves and vests, iced neck wraps, breathable fabrics, moisture-wicking undergarments, shirts and socks, and UV-resistant tops and cover-ups can help minimize the symptoms of hot flashes as they occur.”
Stay hydrated
Hot flashes often cause sweating, which means your body loses fluids. Drinking plenty of water throughout the day helps you stay cool and replace what you lose. Herbal teas served cold can be soothing, too.
Watch your food and drink triggers
Spicy dishes, hot beverages, and caffeine can all make hot flashes worse for some women. Spicy foods in particular can cause hot flashes due to a chemical called capsaicin, which produces heat. Dr. Sherry notes that, “Capsaicin makes the blood vessels dilate and fill with blood, which causes a warm sensation. Hot flashes and sweating can occur as a result of this phenomenon. Avoiding foods containing capsaicin is one way to avoid hot flashes while eating spicy foods.” This doesn’t mean you have to skip your morning coffee or Taco Tuesdays. Just stick to one cup of coffee and steer clear of jalapeños to keep hot flashes at bay. Keeping a simple food diary for a week or two may help you notice patterns and avoid common triggers.
Limit red wine
While not all alcohol will trigger a hot flash, Dr. Sherry notes that red wine, in particular, can be an issue. “Drinking red wine causes the blood vessels to relax, vasodilate, and expand, making you feel warm or flushed. Some experience intense hot flashes, while others only feel warmer. Limiting the amount of red wine or other alcoholic beverages that cause a similar effect should be part of your hot flash treatment management.”
Try cooling techniques
A splash of cool water on your wrists, neck, or face can calm a hot flash as it starts. Some women use cooling pillows or gel packs for extra comfort, especially at night.
Maintain a healthy weight
Research shows women with a higher body mass index (BMI) often experience more frequent or severe hot flashes. Even small amounts of weight loss can help reduce intensity and improve overall well-being.
Supplements and alternative support
Consider supplements
If you have mild symptoms, you may benefit from some dietary supplements, including soy extracts, rhubarb, and pollen extract. They can be helpful, but it can be difficult to maintain consistent results with them. Some women also benefit from ginseng, maca, cannabinoids, and black cohosh. Typically, these can work well as added support, not as your only treatment. Always talk with your provider before starting supplements, since they may not be safe for everyone and can interact with other medications.
Mind-body therapies
Cognitive behavioral therapy (CBT), mindfulness, or even clinical hypnosis can help. These approaches don’t stop hot flashes, but they can make them feel less disruptive by lowering stress and giving you tools to cope.
Hot flashes making life uncomfortable? See how hormone therapy can help you regain control.
You don’t have to “just deal with it.” If hot flashes are affecting your sleep, mood, or daily life, professional care can help. Talk with a QuickMD doctor today to see if menopause hormone therapy can help you regain control and start feeling like yourself again.
We just launched our Menopause Hormone Therapy Membership in select states, and your first month’s on us. You’ll get to meet with a doctor, ask all your questions, and see if treatment might help.
If you love it and want to keep going, it’s $ 79/month after that, with special member pricing on medication and regular access to your doctor. And if you decide it’s not for you – that’s totally fine too. Get started by booking your free visit now.

